Molecular Pathway Promotes Onset of Alport Glomerular Disease in Mouse Study
Researchers identified a molecular pathway that may contribute to the development of Alport glomerular disease and whose activation may be used as a possible biomarker for the disease, according to a new study.
The study, “Endothelin A Receptor Activation On Mesangial Cells Initiates Alport Glomerular Disease,” was published in the journal Kidney International.
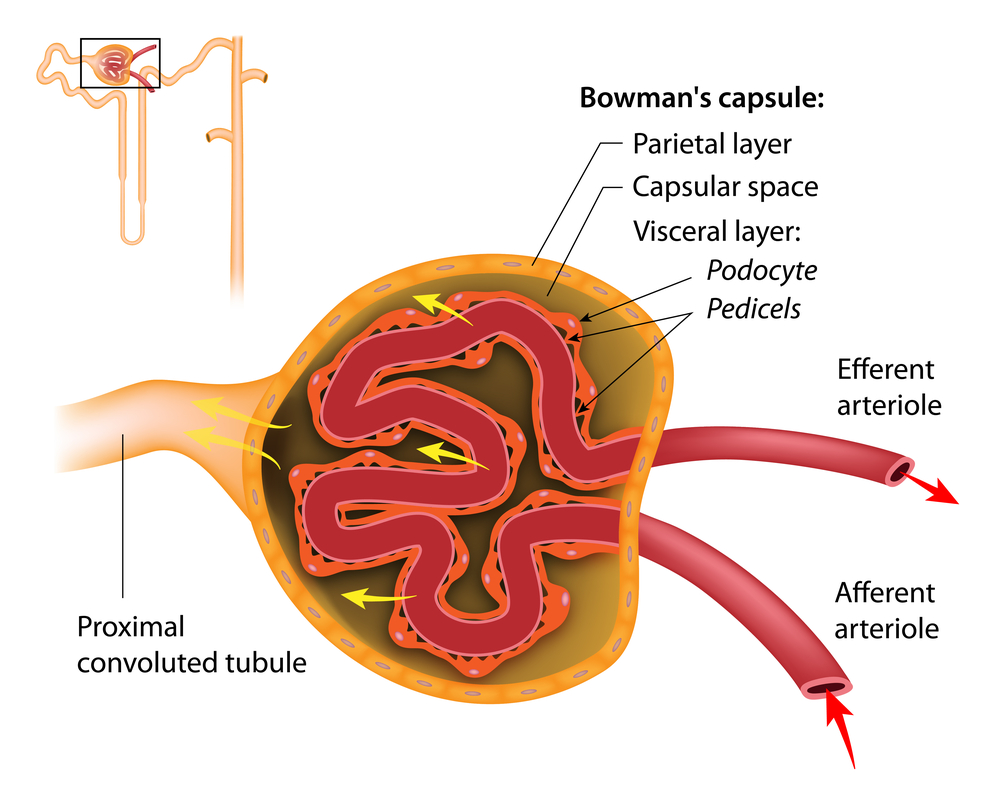
Alport glomerular disease results from changes in the mesangium, a structure associated with capillaries located within the kidney. These changes are mediated by the activation of a molecular pathway that promotes the invasion of mesangial cells into the spaces between capillaries and the accumulation of inflammatory proteins. Together, these events contribute to inflammation in the glomeruli, the structures responsible for the elimination of urine. But their trigger remains unknown.
Researchers hypothesized that ET-1, a protein expressed in the cells lining the glomeruli, could be involved in the initial phases of Alport glomerular disease, as mesangial cells express endothelin A receptors, which are activated by binding to ET-1.
Using mice with Alport glomerular disease, the team observed that ET-1 levels increased before the onset of symptoms, and were further elevated by increases in blood pressure. They also observed that, in mesangial cells cultures, ET-1 binding to endothelin A receptors on the cells’ surface led to the formation of filopodia, structures that help cells move (and possibly invade the spaces between capillaries). However, this effect was blocked when cells were treated with sitaxentan, a molecule that inhibits the activation of these receptors, or with ET-1 inhibitors.
Treating Alport mice with sitaxentan also delayed an increase in proteinuria (presence of proteins in the urine, and a sign of kidney disease), normalized glomerular morphology, prevented mesangial invasion of the glomerular capillaries and normalized levels of inflammatory proteins. The animals also lived longer.
Together, these results supported the idea that ET-1 plays a role in Alport glomerular disease by activating endothelin A receptors on mesangial cells, leading to inflammation.
“Identification of elevated ET-1 levels in the urine of preproteinuric Alport mice suggests that ET-1 may be an early biomarker for Alport renal disease as it has proven to be for other models of [chronic kidney disease],” the researchers wrote. “The development of early biomarkers is currently a priority in the Alport field, as it may provide a sensitive means of monitoring response of emergent therapies.”
Further research is necessary to determine whether ET-1 levels also increase in pre-symptomatic Alport patients as well.







Leave a comment
Fill in the required fields to post. Your email address will not be published.